Patellofemoral instability
Updates to Article Attributes
Patellar instability is the morphologic abnormality in patellofemoral joint, which leads to recurrent patellar dislocations. The patellar dislocates laterally.
Epidemiology
Most patients with patellar instability are young and active individuals, especially females in the 2nd decade. Prevalence is 6-77 per 100,000 population 2.
Pathology
The normal patellofemoral joint has two kinds of stabilizers - active stabilizers (extensor muscles), and passive stabilizers (bones and ligaments):
- bone stabilizers:deep femoral sulcus, high lateral trochlea
- ligament stabilizers:medial patellofemoral retinaculum, medial patellofemoral ligament
The most common mechanism of first-time patellar dislocation is a flexed position of the knee with internal rotation of planted foot with a valgus component.
Anatomical variants of patellar stabilizers are:
- trochlear dysplasia: trochlear joint surface is flattened
- patella alta
- lateralisation of the tibial tuberosity
Secondary factors contributing to patellar instability are femorotibial malrotation, genu recurvatum and ligament laxity (Ehler-Danlos syndrome, Marfan syndrome).
Trochlear dysplasia
Content pending.
Radiographic features
Plain film
The "crossing sign" represents abnormally elevated floor of the trochlear groove rising above the top of the wall of one of the femoral condyles, assessed on lateral radiographs. "Double contour sign" is a double line at anterior aspect of condyles, and seen if medial condyle is hypoplastic. Skyline view can show decreased trochlear depth and large sulcus angle (>150 degree).
MRI
Lateral trochlear inclination, trochlear facet asymmetry, and trochlear depth are used to judge trochlear dysplasia (See images of Case 1).
Classification of trochlear dysplasia (Dejour et al)3
- type A: normal shape of trochlea, but shallow trochlear groove
- type B: markedly flattened or even convex trochlea
- type C: trochlear facet asymmetry, with too high lateral facet, and hypoplastic medial facet
- type D: type C features and vertical link between facets ('cliff pattern')
Lateral trochlear inclination
The most superior section showing trochlear cartilage is selected for this measurement. The inclination is the angle formed between the plane of the lateral trochlear facet subchondral bone and a tangential line through posterior femoral condyles (See images from Case 1). An angle of less than 11 degrees is considered abnormal.
Trochlear facet asymmetry
This is the ratio of medial trochlear facet width to lateral trochlear facet width and measured in the axial plane (As described in images from Case 1). A ratio of less than 0.4 is considered abnormal (ie. it is abnormal if the medial facet is less than 40% the width of the lateral facet).
Trochlear depth
This measures the inset depth of the trochlear groove (sulcus) relative to the mean of the medial and lateral femoral condyle outsets. It is determined by axial imaging at the same level as the trochlear facet asymmetry. A trochlear depth of less than 3mm is considered abnormal.
Patella alta
Patella alta (or a high riding patella) describes a situation where the position of the patella is considered high. See patella alta article for description of the Insall-Salvati ratio.
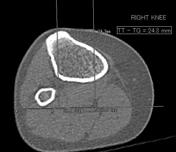
Distance from the tibial tubercle to the trochlear groove
Patella alta
Associated radiological features of patellar instability
- knee joint effusion
- medial patellofemoral ligament tear
- bone contusion in patella and lateral condyle
- osteochondral defects in patella
- edema/hemorrhage of vastus medialis
- intra-articular loose bodies
- internal derangement of knee
Treatment and prognosis
Nearly half of the patients with first-time dislocation will sustain recurrent dislocation after conservative management. Chronic patellar instability, if not treated, may lead to severe arthritis and chondromalacia patellae. Aim of the surgery is to repair the knee damage caused by patellar dislocation and to correct the primary anatomical anomaly. Surgical modalities are:
- medial patellofemoral ligament reconstruction
- trochleoplasty
- medialization of tibial tuberosity
- medial capsular plication
-<p><strong>Patellar instability </strong>is the morphologic abnormality in patellofemoral joint, which leads to recurrent patellar dislocations.</p><h4>Epidemiology</h4><p>Most patients with patellar instability are young and active individuals, especially females in the 2nd decade. Prevalence is 6-77 per 100,000 population <sup>2</sup>.</p><h4>Pathology</h4><p>The normal patellofemoral joint has two kinds of stabilizers - active stabilizers (extensor muscles), and passive stabilizers (bones and ligaments):</p><ul>- +<p><strong>Patellar instability </strong>is the morphologic abnormality in patellofemoral joint, which leads to recurrent patellar dislocations. The patellar dislocates laterally.</p><h4>Epidemiology</h4><p>Most patients with patellar instability are young and active individuals, especially females in the 2nd decade. Prevalence is 6-77 per 100,000 population <sup>2</sup>.</p><h4>Pathology</h4><p>The normal patellofemoral joint has two kinds of stabilizers - active stabilizers (extensor muscles), and passive stabilizers (bones and ligaments):</p><ul>
-</ul><h5>Lateral trochlear inclination</h5><p>The most superior section showing trochlear cartilage is selected for this measurement. The inclination is the angle formed between the plane of the lateral trochlear facet subchondral bone and a tangential line through posterior femoral condyles (<em>See images from Case 1</em>). An angle of less than 11 degrees is considered abnormal.</p><h5>Trochlear facet asymmetry</h5><p>This is the ratio of medial trochlear facet width to lateral trochlear facet width and measured in the axial plane (<em>As described in images from Case 1). </em>A ratio of less than 0.4 is considered abnormal (ie. it is abnormal if the medial facet is less than 40% the width of the lateral facet). </p><h5>Trochlear depth</h5><p>This measures the inset depth of the trochlear groove (sulcus) relative to the mean of the medial and lateral femoral condyle outsets. It is determined by axial imaging at the same level as the trochlear facet asymmetry. A trochlear depth of less than <strong>3mm</strong> is considered abnormal. </p><h5>Patella alta</h5><h5>Distance from the tibial tubercle to the trochlear groove</h5><p><a href="/articles/patella-alta">Patella alta</a> is being advocated as one of the accurate measures of patellar instability. For this measurement, axial images at these levels are superimposed by increasing the MIP thickness. The distance from the tibial tuberosity to the trochlear groove is measured parallel to the tangential line through posterior femoral condyles. A distance of less than 15mm is considered normal, 15 to 20mm is considered borderline and a distance greater than 20mm is considered abnormal.</p><h5>Associated radiological features of patellar instability</h5><ul>- +</ul><h5>Lateral trochlear inclination</h5><p>The most superior section showing trochlear cartilage is selected for this measurement. The inclination is the angle formed between the plane of the lateral trochlear facet subchondral bone and a tangential line through posterior femoral condyles (<em>See images from Case 1</em>). An angle of less than 11 degrees is considered abnormal.</p><h5>Trochlear facet asymmetry</h5><p>This is the ratio of medial trochlear facet width to lateral trochlear facet width and measured in the axial plane (<em>As described in images from Case 1). </em>A ratio of less than 0.4 is considered abnormal (ie. it is abnormal if the medial facet is less than 40% the width of the lateral facet). </p><h5>Trochlear depth</h5><p>This measures the inset depth of the trochlear groove (sulcus) relative to the mean of the medial and lateral femoral condyle outsets. It is determined by axial imaging at the same level as the trochlear facet asymmetry. A trochlear depth of less than <strong>3mm</strong> is considered abnormal. </p><h5>Patella alta</h5><p>Patella alta (or a high riding patella) describes a situation where the position of the patella is considered high. See <a href="/articles/patella-alta">patella alta</a> article for description of the Insall-Salvati ratio.</p><h5>Distance from the tibial tubercle to the trochlear groove</h5><p>The distance from the tibial tubercle to the trochlear groove (<em>TT-TG distance</em>) is being advocated as one of the accurate measures of patellar instability. For this measurement, axial images at these levels are superimposed by increasing the MIP thickness. The distance from the tibial tuberosity to the trochlear groove is measured parallel to the tangential line through posterior femoral condyles (<em>as described in images from Case 5)</em>. A distance of less than 15mm is considered normal, 15 to 20mm is considered borderline and a distance greater than 20mm is considered abnormal. The distance has been shown to be slightly less when measured on MRI than CT <sup>4</sup>.</p><h5>Associated radiological features of patellar instability</h5><ul>
References changed:
- 6. Hinckel B, Gobbi R, Filho E et al. Are the Osseous and Tendinous-Cartilaginous Tibial Tuberosity-Trochlear Groove Distances the Same on CT and MRI? Skeletal Radiol. 2015;44(8):1085-93. <a href="https://doi.org/10.1007/s00256-015-2118-4">doi:10.1007/s00256-015-2118-4</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/25708103">Pubmed</a>
Image 11 CT (non-contrast) ( update )







 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.